Fatigue, Chronic Fatigue, Chronic Fatigue Syndrome: Same Same, but Different?
Everyone gets tired, some people experience fatigue. Chronic Fatigue is more than that. It’s chronic! Fatigue, not alleviated by rest (or coffee!). To be considered Chronic, the ongoing fatigue would be present for at least 4-6 months[i].
Chronic Fatigue is associated with numerous conditions: lymes disease, mental illnesses, insomnia, adult-ADHD/ADD, hypothyroidism, cancer (particularly post treatment), medication side-effects, rheumatoid arthritis, post-stroke, post-surgery, chronic pain, Chron’s Disease and Lupus… just to name a few.
Chronic Fatigue Syndrome
Chronic Fatigue Syndrome, is also referred to as Myalgic Encephalomyelitis (My = muscle, Algic = Pain, Encephalo = Brain, Mye = Spinal cord, Itis = Inflammation). More recently it has been referred to as Systemic Exertion Intolerance Disease. It is currently considered a neurological disorder, but the symptoms also include immune, gastro-intestinal and metabolic dysfunction.
It is often preceded by a flu-like disease (they get sick with the flu and then never seem to recover), and sometimes a prolonged period of adverse stress – physical or psychological.1 Chronic fatigue symptoms often reflect the symptoms of the preceding illness.[i]
The severity is extreme, from sufferers ‘sort of coping’ to being bed ridden and needing care. Being an “invisible illness,” adding to the stress of the physical symptoms endured, they are often met with misunderstanding and judgement because “well I’m tired too”. The condition results in a decreased ability to perform usual activities (such as household duties, hobbies and even work); they do not have the energy to do what they used to be able to! This all comes with a decreased confidence in recovery due to fear of exacerbation.
Diagnosis
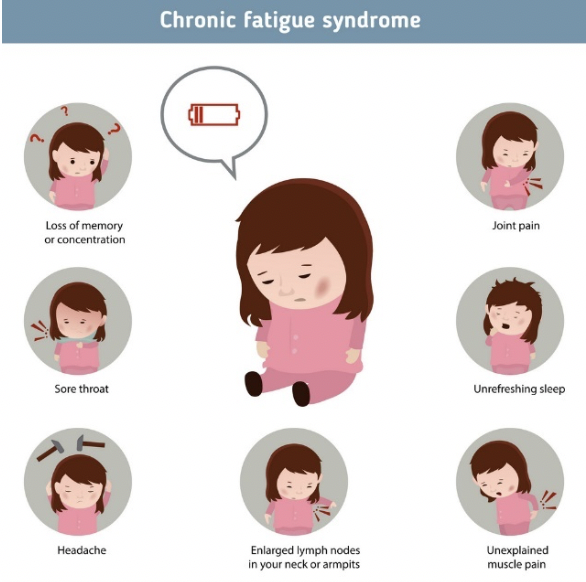
There are also many other symptoms that are associated with CFS including: IBS, bloating, nausea, chest pain, night chills/sweating, shortness of breath, visual disturbances (blurred vision, light sensitivity, eye pain, dry eyes), allergies or sensitivities to foods, alcohol, odours, chemicals, medications, noise, poor ability to remain upright, irregular heart rate, dizziness and mood swings. 2
Understandably, 48% of clinicians do not feel confident making a ME/CFS diagnosis and 67% believe it is the most difficult condition to diagnose.[ii]
Although diagnosis is currently symptom and history based, there is often new research coming out attempting to find objective measures to diagnose and understand aetiology. Here’s a few we’ve come across recently:
- A blood test which measures the immune cells’ response to stress[i]
- CFS may be an autoimmune disease[ii]
- A blood test which measures specific cytokines associated with inflammation[iii] (cytokines are proteins that act as “intercellular chemical messengers,” impacting the cellular behaviour of numerous cells and therefore their physiological processes, including immune cells)
- Researcher’s from Griffith University are looking into diagnostic tests to measure ability of calcium ions to enter cells[iv]
- CFS patients have been found to have a significantly different microbiome in their mouth compared to healthy controls![v]These particular bacteria are associated with amino acid and energy metabolism.
Treatment
There’s also ongoing research to find optimal treatment for CFS. At the moment the common modalities include:
- Pharmacological (anti-depressants)
- CBT
- Pacing
- Graded Exercise Therapy
CBT is also hotly debated1but seems most effective when combined with GET with suggestions that recovery is possible.[i]
DID YOU SAY EXERCISE?!
Won’t Exercise make it worse?
Can it? Yes.
Will it? Not necessarily
Exercise, specifically, Graded Exercise Therapy (GET), with Cognitive Behavioural Therapy (CBT) and Pacing strategies, are the most common treatment modalities.
GET is as it sounds: establishing a physical activity baseline and progressively increasing the grade through duration, and then intensity.7
The PACE Trial (“Pacing, graded Activity and Cognitive behavioural therapy; a randomised Evaluation”) has been the biggest study to date being a 5 year long study with 641 patients. It was published in The Lancet in 2011 and showed a combination of GET and CBT to be superior. GET is recommended by most health body’s and Fatigue Centres but has received a lot of criticism, in fact there’s been a bit of drama with publications attempting to devalue the PACE Trial’s outcomes. The arguments appear to be based on the selection criteria (i.e. definition of the disease) and the statistical analysis methods. However PACE published a rebuttal earlier this year[i]defending their results with specific details to the criticisms.
The Cochrane Review(recognised as the highest standard in evidence-based health care) states that “Patients with CFS may generally benefit and feel less fatigued following exercise therapy, and no evidence suggests that exercise therapy may worsen outcomes”.[ii]
Before we put you to sleep with too much information, we’ll wrap it up here! But stay tuned for PART 2 where you’ll learn about…
- Other treatment approaches, including
- Our unique approach to chronic fatigue syndrome

Biara Webster
Exercise Physiologist and Writer
Follow Specialised Health
- Geraghty (2019), The ‘cognitive behavioural model’ of chronic fatigue syndrome: a flawed model, Health Psychology Open, January-June 2019: 1-14– Thanks to Alice, H.S Fung for sharing this link on her LinkedIn!
- N Butler (2018), Chronic Fatigue Syndrome Pacing & Exercise, ESSA Webinar
- DJ Borah (2013), Chapter160 chronic fatigue syndrome: a review, medical updates, The Association of Physicians India
- Emerge.org.au
- L Chu et al., (2018), Deconstructing post-exertional malaise in myalgic encephalomyelitis/chronic fatigue syndrome: a patient-centered, cross-sectional survey, PLos ONE 13(6): e0197811.
- A Chronic Fatigue Blood Test Looks Increasingly Promising, But It’s Still Early Days (2019),https://www.sciencealert.com/a-blood-test-for-chronic-fatigue-looks-promising-but-it-s-too-early-to-be-certain– Thanks to June Khawfor sharing this on LinkedIn!
- F Sotnzy et al., (2018), Myalgic encephalomyelitis/chronic fatigue syndrome – evidence for an autoimmune disease, Autoimmunity Reviews, Vol 17, Issue 6, pp 601-609
- New Research Renews Hope for Chronic Fatigue Diagnostic Test (2017) https://www.healthline.com/health-news/chronic-fatigue-diagnostic-test#2
- Your disease is real: breakthrough in diagnosis of chronic fatigue syndrome(2018),https://www.abc.net.au/triplej/programs/hack/breakthrough-in-diagnosis-of-chronic-fatigue-syndrome/10188210
- Wang et al. (2018), Chronic fatigue syndrome patients have alterations in their oral microbiome composition and function, PLoS One13 (9)
- White et al., (2013), Recovery from chronic fatigue syndrome after treatments given in the PACE trial,. Psychological Medicine, 43, 2227-2235.
- M Sharpe (2019) The PACE trial of treatment for chronic fatigue syndrome: a response to WILSHIRE et al, BMC Psychology, 2019, 7:15
- L Larun et al. (2017), Exercise therapy for chronic fatigue syndrome, Cochrane Systematic Review


